Respiratory rate, the number of breaths per minute, is a key vital sign that reflects your respiratory and metabolic function. It’s highly sensitive, responding quickly to stress, illness, and physical activity, which makes it a critical marker of your physiological state [1], [2].
In exercise, breathing rate provides deep insight into fitness, recovery, and the transition between training zones (like the ventilatory thresholds). It also plays a foundational role in autonomic regulation through its influence on heart rate variability (HRV), particularly via respiratory sinus arrhythmia [3].
Because your breathing rate so profoundly affects HRV metrics, monitoring it is essential. It adds invaluable context that is necessary for accurate HRV analysis and exercise assessment [4].

How breathing can distort your HRV: The frequency-domain problem
Respiration and HRV are tightly connected through a natural pattern called respiratory sinus arrhythmia, where your heart rate increases as you inhale and decreases as you exhale [3]. This effect is driven by the parasympathetic nervous system (your “rest-and-digest” system) and is most pronounced during slow, relaxed breathing.
Because of this link, your breathing rate directly influences HRV metrics. This is especially true for high frequency (HF) power, which is a core metric used to measure parasympathetic activity. The HF band is traditionally defined as 0.15 to 0.4 Hz, which corresponds to a breathing rate of 9 to 24 breaths per minute.
Here is the critical issue: If your breathing rate drops below this range, the HF power metric becomes misleading.
When you breathe slower than 9 breaths per minute (<0.15 Hz), the respiration-related heart rate modulation shifts out of the HF band and into the Low-Frequency (LF) band. This makes the HF power value artificially low, or even zero, making it meaningless for evaluating your recovery status.
Furthermore, purposeful deep breathing exercises are well-known to stimulate the parasympathetic nervous system, resulting in an immediate and significant increase in the overall magnitude of heart rate variability. It’s crucial to understand that this is an acute effect caused by the breathing pattern itself—a “respiratory-driven enhancement” of vagal modulation [3]. This immediate spike should not be confused with an instant reduction in cumulative stress or a fundamental change in your underlying, baseline recovery state.
Breathing as a marker of exercise intensity
In exercise physiology, respiratory rate is invaluable for assessing cardiorespiratory efficiency and training intensity. As you exert yourself, your breathing rate increases to meet the body’s demand for oxygen and the need to clear carbon dioxide.
Monitoring respiratory rate alongside heart rate and HRV gives a complete view of the body’s response to physical activity. It is a sensitive indicator of physical effort, increasing in parallel with blood lactate levels and perceived exertion [5].
Critically, your breathing pattern can indicate ventilatory thresholds (VT), such as the transition from aerobic to anaerobic metabolism [6]. Identifying this threshold is essential for optimizing training intensity.
In Kubios software, respiratory rate is a key component in the non-invasive estimation of your VT from ECG or RR-interval data. The Kubios VT algorithm detects this shift by analyzing respiratory rate alongside heart rate and HRV dynamics, enabling accurate VT assessment without the need for gas exchange measurements.
How Kubios estimates respiratory rate (without extra sensors)
Kubios HRV software products feature scientifically validated algorithms that estimate respiratory rate directly from your existing heart rate variability data. This eliminates the need for separate respiratory sensors (like a chest strap or mask) and makes physiological monitoring far more accessible.
Two estimation methods are available:
- ECG + RR Method: This method combines the ECG waveform and RR interval data to detect respiration-induced changes. It provides the highest accuracy and is utilized always when ECG waveform data is available.
- RR-Only Method: This method estimates respiratory rate from the RR interval time series alone. It is ideal when an ECG waveform data is not available, which is the case for most consumer-grade heart rate wearables.
These methods were validated in both resting and exercise conditions [7]. The ECG + RR method showed strong agreement with reference signals (R = 0.92 during exercise). The RR-only method also performed very well, especially during exercise (R = 0.88). These results confirm that both algorithms provide reliable respiratory rate estimates for accurate, integrated analysis.
For more details about the Kubios respiratory rate estimation algorithm, please read the “Accuracy of Kubios HRV software respiratory rate estimation algorithms” white paper.
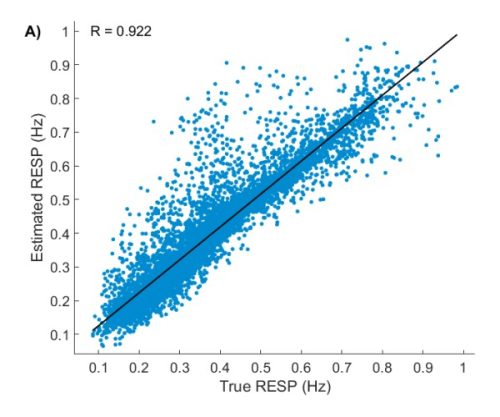
Figure: Accuracy of Kubios respiration rate estimate for exercise data, using both ECG and RR data.
Putting it all together: Practical tips for using respiratory rate
How to enhance your HRV assessments:
- For general HRV analysis: To ensure accurate interpretation, always include the Kubios validated respiratory rate estimate in your analysis. It is critical to confirm that the breathing rate is within the high-frequency band (0.15–0.4 Hz) before reporting frequency-domain parameters like LF and HF power.
- For daily readiness: When using the Kubios HRV App for your morning readiness, maintain consistency and avoid intentionally changing your breathing rate. The goal is to capture your natural, resting state. Check the estimated respiratory rate in the app afterward to ensure it’s at a similar level each morning, as this consistency is key to reliable long-term HRV trends.
How to empower your exercise analysis:
- Evaluate internal load: Kubios’ training analysis displays your respiratory rate trend across the entire workout. It also provides time spent in respiratory rate zones (light, moderate, hard) to give insight into the internal load distribution. If a “light” session shows significant time in “hard” respiratory zones, it may be a sign of accumulated fatigue or insufficient recovery.
- Check post-exercise recovery: A clear and rapid decrease in respiratory rate during your cool-down (along with heart rate) indicates efficient autonomic recovery and good cardiovascular fitness.
Conclusion
Respiratory rate is a key physiological signal that provides essential context for both autonomic and exercise-related assessments. Very low breathing rates, in particular, can distort HRV metrics, making respiratory estimation essential for an accurate interpretation of your HRV results.
Kubios HRV software solves this by integrating validated respiratory rate estimation directly from your ECG or RR data. This enhances the value of your HRV analysis in both rest and exercise, supporting more informed decisions in health, performance, and recovery monitoring.
Frequently asked question (FAQ)
Why is respiratory rate important in HRV analysis?
Respiratory rate is crucial because it directly influences HRV through a process called respiratory sinus arrhythmia (RSA). Very low breathing rates (e.g., <9 breaths/min) can distort key metrics, particularly by shifting power out of the high frequency (HF) band. This can make your HF power appear artificially low, leading to a misinterpretation of autonomic nervous system balance.
Can respiratory rate be estimated from ECG or RR data without a dedicated breathing sensor?
Yes. Kubios software includes validated algorithms that estimate respiratory rate directly from your heart rate data. It does this by analyzing either respiration-induced changes in the ECG waveform (if available) or patterns in the RR interval time series, eliminating the need for a separate respiratory sensor.
How accurate is respiratory rate estimation in Kubios software?
The accuracy is very high and has been scientifically validated in both resting and exercise conditions. Our ECG-based method is the most precise (correlation R = 0.92 during exercise), but the RR-only method also performs very well, ensuring you get reliable data for your analysis.
What is the benefit of monitoring respiratory rate during exercise?
Respiratory rate is a sensitive marker of physical effort and provides deeper insight into your “internal load.” It increases with intensity, and its pattern can reflect metabolic transitions, like the ventilatory threshold (VT). Kubios uses this data to help you non-invasively assess your training zones.
If I do slow breathing exercises, does the high HRV mean my stress is gone?
Not exactly. Slow, deep breathing directly stimulates your parasympathetic nervous system, causing an immediate, temporary increase in your HRV. This is an acute effect of the breathing pattern itself, not an instant reduction of your cumulative life stress. However, regular breathing exercises along with other relaxation techniques and physical activity, are a great way to enhance recovery and manage stress.
References
- Kral TRA, Weng HY, Mitra V, Imhoff-Smith TP, Azemi E, Goldman RI, Rosenkranz MA, Wu S, Chen A, and Davidson RJ. Slower respiration rate is associated with higher self-reported well-being after wellness training. Scientific Reports, 13 (15953), 2023.
- Cretikos MA, Bellomo R, Hillman K, Chen J, Finfer S, and Flabouris A. Respiratory rate: the neglected vital sign. Med J Aust, 188(11): 657–659, 2008.
- Grossman P and Taylor EW. Toward understanding respiratory sinus arrhythmia: Relations to cardiac vagal tone, evolution and biobehavioral functions. Biol Psychol, 74(2):263–285, 2007.
- Laborde S, Mosley E, and Thayer, JF. Heart rate variability and cardiac vagal tone in psychophysiological research – Recommendations for experiment planning, data analysis, and data reporting. Front Psychol, 8, 213, 2017.
- Nicolò A, Massaroni C, and Passfield L. Respiratory frequency during exercise: the neglected physiological measure. Front Physiol, 8, 922, 2017.
- Cross TJ, Morris NR, Schneider DA, and Sabapathy S. Evidence of break-points in breathing pattern at the gas-exchange thresholds during incremental cycling in young, healthy subjects. Eur J Appl Physiol, 112(3):1067–76, 2012.
- Lipponen JA and Tarvainen MP. Accuracy of Kubios HRV software respiratory rate estimation algorithms. Kubios white paper, June 2021.
